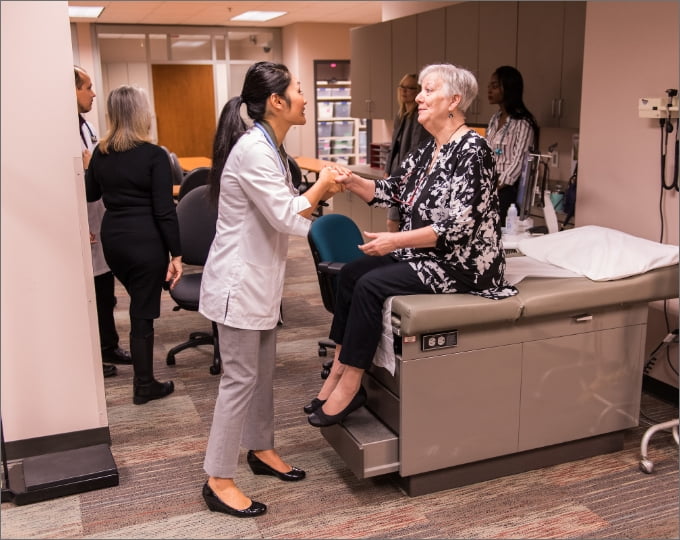
Mentorship and Preceptorship in Nursing
May 7, 2026Nurses rely on guidance throughout every stage of their careers, but not all guidance serves the same purpose. Mentorship and preceptorship often work alongside each other, but they are not interchangeable roles.
Understanding the difference between a preceptor vs. mentor matters for students entering clinical training as well as nurses developing long-term careers. Generally speaking, preceptors focus on hands-on clinical instruction, while mentors focus on career development and professional growth.
What’s the Difference Between a Mentor and a Preceptor?
The difference between preceptorship and mentorship in nursing involves the purpose of these roles in the education and healthcare systems. Structure and timing make a big difference in understanding which title and role is fitting.
For example, a mentor is typically focused on helping current nurses with career and professional growth, whereas a preceptor is committed to helping nursing students develop skills in the clinical setting. Mentors may be longer-term relationships, whereas preceptors are frequently assigned for shorter-term clinical rotations.
Most nurses and nurse practitioners will work with both preceptors and mentors at different points during their education and career. Preceptors and mentors contribute in different but complementary ways to a nurse’s overall development. Nurses thinking about giving back to the profession can move forward with confidence by understanding the difference between a preceptor vs. mentor.
What Is a Nurse Mentor?
A nurse mentor is an experienced professional who offers ongoing support and perspective. According to the American Nurses Association, mentors help mentees:
- Enjoy career satisfaction
- Refine specialty and problem-solving skills
- Work through role transitions
- Develop as a leader
Mentorship can happen in academic or clinical settings. Faculty may mentor students during a program, while experienced nurses and nurse practitioners often mentor colleagues through employment connections. Mentors make a meaningful difference for nurses by providing trusted help and close communication between colleagues.
What Can Nurses Expect From a Mentor?
A mentor relationship is about helping develop advanced practice nursing skills and decision-making over time. The primary purpose is not to evaluate performance for the assignment of grades. Instead, mentors help nurses and nurse practitioners make sense of their experiences. Sometimes the greatest contribution of a mentor is the presence they provide.
Nurses of all levels can expect a mentor to:
- Provide honest yet supportive guidance based on real experience
- Listen and help process thoughts in difficult or overwhelming situations
- Share lessons learned (including mistakes and setbacks)
- Help the mentee identify their strengths
- Encourage personal and professional reflection
In most cases, a mentorship relationship grows over time. However, mentorship may be shorter-term. This often depends on the stage of the career and may transition when there is a specialty change.

Types of Mentorship in Nursing
Mentorship is often structured with flexibility and can take different forms depending on the mentorship setting, goals of those involved, and the experience levels of the mentor(s) and mentee(s).
Formal mentorship programs are frequently offered by hospitals, universities, or professional organizations. Mentors and mentees might be paired based on goals or specialty areas. There may be set timelines, regular check-ins, and defined outcomes like leadership milestones or career advancement.
Informal mentorship relationships develop naturally between colleagues with shared experiences. A nurse practitioner may seek guidance from someone they respect or connect with over time. Informal mentorship is usually based on trust and ongoing conversation.
Each type of mentorship serves the purpose of supporting steady, long-term development. The right format often depends on what the nurse needs at a particular point in their career. Other examples might include:
- Peer mentorship between nurses at similar stages of their careers
- Group mentorship where one mentor works with multiple mentees
- Situational mentorship with specific and focused goals/skills at the forefront
New graduates may support each other peer-to-peer as they move from school into practice. Even though peer mentors may not have more experience than one another, the mentorship is unique because of shared experience. Group mentorship creates discussion opportunities and allows nurses to have exposure to diverse perspectives.
Some mentorship relationships are focused on a specific, short-term goal, such as preparing for a certification exam or developing a particular skill, such as trauma-informed care. Most (if not all) of these mentorship situations may occur in academic or professional development settings.
What is a Nurse Preceptor?
To answer the question, what is a nurse preceptor, you can think of a nurse who teaches field experiences for students or new hires. For nurses and nurse practitioners, these are clinical rotations in real-world settings with direct patient interaction.
A nurse preceptor is an experienced clinician who supervises students or new nurses and nurse practitioners in a clinical setting. Their role is to help bridge the gap between textbook or simulation knowledge and actual practice. Preceptors work directly with students and also collaborate with clinical supervising faculty to help ensure education and remedial efforts are effective.
Preceptors also orient new hires to the clinical setting by working alongside them throughout the onboarding process. Together, they see patients, practice essential clinical skills, document care, and collaborate with other members of the healthcare team. As the new nurse practitioner gains confidence and competence, the preceptor gradually increases their independence while working with the manager and/or nurse educator to ensure learning needs are met and expectations are achieved.
Nurse preceptors:
- Teach clinical skills during patient care
- Supervise and guide clinical decisions
- Give practical feedback
- Evaluate progress and readiness for independent practice
Preceptorships are usually somewhat structured and time-specific, with a defined practice setting and number of hours. They are connected and aligned with specific learning objectives set by the academic program. Preceptors often work closely with faculty or managers in an employment setting who oversee and evaluate the clinical experience.
Preceptor Qualifications in Nursing
Preceptors are carefully vetted to ensure they meet specific qualifications. While requirements vary by state and program, nurse preceptors may include experienced physicians, physician assistants, nurse practitioners, and registered nurses who are prepared to guide students or new hires through hands-on clinical learning and professional transition.
While requirements vary by state and program, most nurse preceptors typically have:
- An active, unencumbered RN or APRN license (at minimum, the equivalent of the employment or educational program of the preceptorship)
- Clinical experience in their specialty area (often at least 1 to 2 years)
- Current knowledge of evidence-based practice and standards of care
- Strong communication and teaching skills
Many universities and employers offer a brief training orientation for new preceptors. Precepting is an opportunity to directly shape the next generation of nurses.
What Can Students Expect From a Preceptor?
A preceptor relationship is usually focused on patient care, skill development, and safe progression toward independence while a student is in an educational program of study. Preceptors evaluate student performance based on clinical standards and program expectations.
Students can expect a preceptor to:
- Demonstrate clinical skills and supervise hands-on practice
- Intervene when needed for safety
- Ask questions that test clinical reasoning and decision-making
- Give feedback during or after patient encounters
- Gradually increase responsibility as competence grows
Preceptors are distinct from mentors because they are not primarily coaches or long-term career advisors. Students can expect a preceptor to ensure they can safely translate classroom knowledge into real clinical practice.
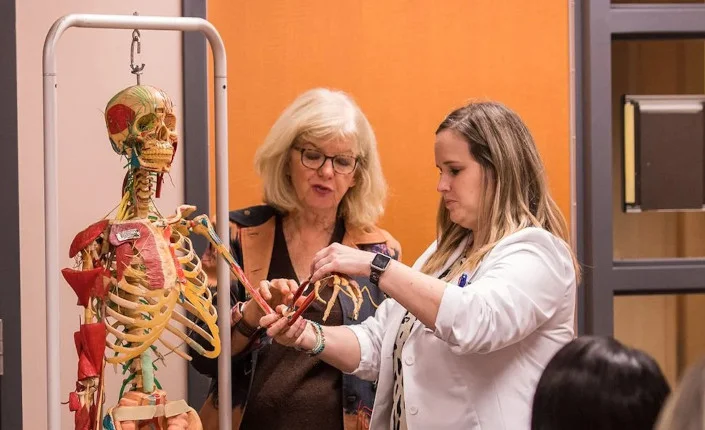
Why Mentorship and Preceptorship Both Matter
Mentorship and preceptorship are both essential to nursing development. They promote teamwork in nursing while focusing on safe and effective practice. Preceptors and mentors both contribute to:
- Development of clinical skills
- Greater confidence in professional environments
- Support for critical thinking while managing stress
While preceptors focus on clinical teaching in structured school-related or employment settings, many nurses continue to seek guidance beyond those experiences. This is where mentorship becomes equally important. Together, preceptorship and mentorship create a more complete support system.
Qualities of Effective Mentors and Preceptors
Strong mentors and preceptors are intentional in how they teach and support nurses at different stages of development. They are skilled communicators who know how to translate knowledge into learning.
Important qualities for effective preceptors and mentors include:
- Willingness to invest time
- Strong clinical experience
- Openness to different perspectives
- Ability to create a supportive learning environment
Effective mentors and preceptors make time for teaching even in busy clinical environments. For example, a preceptor may pause after a patient interaction to walk a student through what went well and what could be improved, rather than waiting until the end of the shift.
When giving feedback, effective preceptors and mentors guide in ways that are specific and able to be implemented. Experience allows them to connect theory to practice. For instance, a mentor with years of intensive care unit (ICU) experience can help a nurse understand how the early signs of patient decline may present differently in real patients compared to textbook examples.
Good mentors and preceptors remain open to questions and discussion. A student may suggest an approach based on recent classroom learning, and the preceptor may explore how that approach fits into the bigger conversation of evidence-based practice and nursing research. Mentors and preceptors also recognize when encouragement is needed.
Becoming a Mentor or Preceptor
Many nurses become mentors or preceptors as they develop experience and a greater desire to help others through what they have also learned. Serving as a mentor or preceptor allows you to:
- Give back to the profession
- Support future nurses
- Strengthen your leadership skills
- Contribute to better patient care
Mentorship and preceptorship are rewarding, meaningful roles. You can find opportunities through healthcare organizations, academic programs, and professional associations. If you are interested in precepting, many universities partner with experienced nurses for recurring rotations with different students.
Learn from Experienced Leaders at Texas Woman’s University
Preceptorship is a core part of the graduate nursing curriculum at Texas Woman’s University (TWU). Students complete supervised clinicals with qualified preceptors, applying knowledge in real-world settings to grow more confident and learn professionalism in practice. The nurse practitioner program also offers clinical placement support to help students find appropriate sites and preceptors.
If you’re ready to take the next step in advancing your nursing career, TWU offers an online Master of Science in Nursing - Family Nurse Practitioner (MSN-FNP) program that combines didactic preparation with clinical instruction by quality faculty and preceptors.